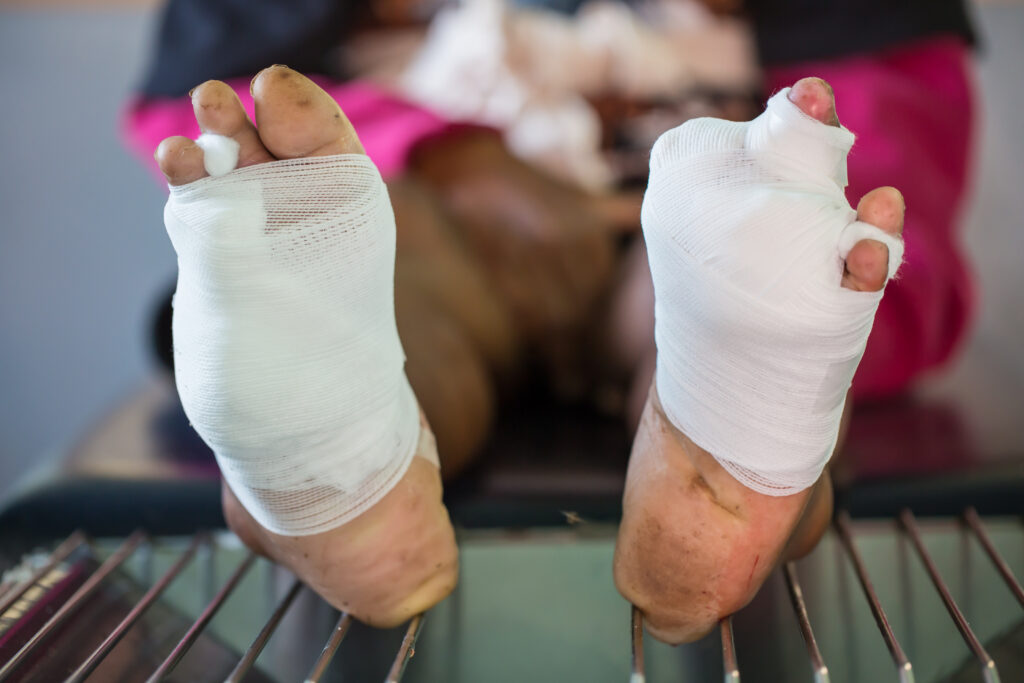
Representing the victims of burn injuries – explaining the treatment of burn injuries.
Burn injuries present complex issues, throughout his career representing people who have suffered burn injuries, Kevin Coluccio has gained a wealth of knowledge and experience in how to best understand and present these types of claims.
The classifications of burns are as follows:
First-degree burns (superficial) affect only the epidermis or outer layer of skin. The first-degree burn site appears red, painful, dry, and with no blisters. An example is a mild sunburn. Long-term tissue damage is rare and usually consists of an increase or decrease in skin color.
Second-degree burns(partial thickness) burns involve the epidermis and part of the dermis layer of skin. Second degree burns appear red, blistered, and may be swollen and painful.
Third-degree burns (full thickness) destroy the epidermis and dermis. Third-degree burns may also damage the underlying bones, muscles, and tendons. Third-degree burns appear white or charred. With third-degree burns, there is no sensation in the area because the nerve endings are destroyed.
Burns are considered major injuries and require hospitalization and extensive rehabilitation when they affect 10 percent of a child’s body and 15 to 20 percent of an adult’s body.
As a general outline, the following provides an overview of how burns are medically treated.
During the early phase of management, therapy is directed primarily toward combating shock and its adverse effects, relief of pain, and prevention of respiratory complications. Burn injuries are considered some of the most painful injuries that can be suffered.
Shock is prevented or reversed by intravenous administration of large amounts of fluids, plasma, or plasma substitutes and, on occasion, whole blood. Severely burned patients may require as much as 10 to 12 liters of intravenous fluids during the first 24 hours after injury in contrast to the normal daily requirement of 2 to 3 liters.
Generally, the initial or shock phase of massive fluid loss from the circulation usually persists during the first 48 hours after injury. Fluid loss is greatest during the first 12 hours. This is a critical time for those suffering from burn injuries.
Therapy for the three to four weeks following the shock phase of burn injury is directed primarily toward the prevention of serious infection in the burn wounds, removal of dead tissue, and obtaining early healing of the wounds. Infections can often occur without proper treatment and care.
Burns involving the entire circumference of the trunk or extremities are usually best managed by what is called the bulky occlusive dressing technique. With this technique, dressings are changed every three days until healing is complete and areas of the burns are ready for grafting.
Early operative excision and skin grafting of third-degree burn areas are most applicable to burns of a small extent and burns of the hands. Due to the difficulty of the procedure, extensive burns are usually not well-suited to management by the technique.
The areas of third-degree burn are not ready for grafting for three to four weeks after burning.
In dermabrasion, the surgeon scrapes away the outermost layer of skin with a rough wire brush or a burr containing diamond particles attached to a motorized handle. In dermaplaning the surgeon uses a dermatome, the same type of instrument used by burn surgeons to obtain skin for grafting.
It is during the initial three-to-four-week period following an injury that infection, the major threat to life, exists. Prevention of invasive bacterial infection is the most difficult task facing the physician caring for a burned patient. Under normal conditions, pathogenic bacteria are unable to penetrate the protective external barrier provided by intact, unwounded skin. This important protective function of the skin is lost, however, when full-thickness skin injury due to burns has occurred. Bacteria may rapidly proliferate and penetrate the layer of dead skin often resulting in fatal bloodstream invasion. Once an invasive infection has occurred in the burn wound, antibiotic therapy is usually ineffectual, and the outcome is fatal in most cases.
The length of hospitalization depends on many factors. In addition to the severity of the burn injury, these factors include whether the person suffered lung injury from inhaling smoke or chemicals and whether the person had pre-existing medical problems, such as heart disease.
There are three phases in the formation of a scar. In the first, phase, which lasts less than a week, the body begins to remove dead and dying skin tissue, fights infection, and sends cells that will begin the healing process to the burned areas. In the second phase, which takes a few weeks, the body makes collagen fibers to form scar tissue and creates tiny new blood vessels in the injured area. In the final phase, which takes months to years, the scar tissue matures, resulting in a stronger scar. Early surgical removal of dead skin and replacement with skin grafts usually accelerates healing.
The initial treatment of burns is extremely painful. The strongest pain medication cannot control the pain that burn victims experience during the debridement process. The extreme pain that people experience with a recent serious burn slowly improves as the wound heals. Burn patients can experience a feeling of skin tightness, numbness, or a tingling or burning sensation as the skin heals. Because the healed skin tends to be drier than normal skin, it may itch if not kept moist.
Every person suffering burn injuries has an individual journey of recovery that is both intense and painful. The general overview above clearly shows the comprehensive nature of the stages of treatment that burn victims must undergo.
Coluccio Law has represented several victims of serious burns for over 30 years. He brings a great deal of experience and knowledge to his clients who have suffered serious burns. Coluccio Law is available for burn injury consultation.
Recommended Article: What to do if you have Suffered a Burn Injury